Exploring Vagus Nerve Stimulators and Their Impact

Intro
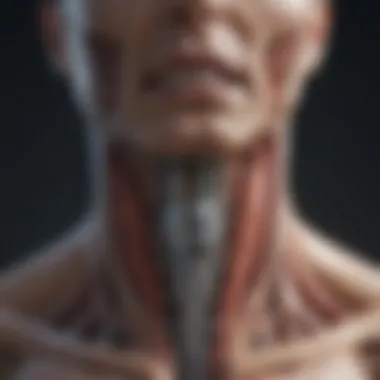
Vagus nerve stimulators have emerged as a vital tool in the realm of neurological therapies. For those unfamiliar, the vagus nerve plays a crucial role in numerous bodily functions, including heart rate, digestion, and immune response. These stimulators interact with this nerve to impact a variety of health conditions, promising innovative solutions to complex medical challenges.
This article will delve into the detailed mechanisms by which vagus nerve stimulators operate, their diverse clinical applications, and the implications they carry for future health initiatives. Researchers, healthcare professionals, and those interested in the evolving landscape of neurological treatments will find the insights presented here particularly relevant as we synthesize knowledge from ongoing studies and clinical practice.
Through this examination, we hope to highlight pivotal research findings, clarify ethical considerations, and guide future inquiries into the use of vagus nerve stimulation.
Research Methodology
Description of Research Design and Approach
The research conducted in this field employs a multi-faceted approach that combines both experimental and clinical studies. Clinical trials often focus on the efficacy and safety of devices designed for vagus nerve stimulation. These trials typically involve randomized controlled designs to minimize bias and maximize the reliability of the results.
In addition to clinical trials, laboratory studies investigate the underlying physiologic mechanisms at play. Understanding the exact pathways and biological responses contributes significantly to the overall knowledge of how vagus nerve stimulation can benefit various health conditions.
Materials and Methods Used in the Study
The studies often use a range of tools and materials, including:
- Vagus nerve stimulators: Devices like the AspireHealth VNS Therapy System, designed for implantation in patients.
- Assessment tools: Scales such as the Hamilton Depression Rating Scale to evaluate patient outcomes.
- Control mechanisms: Placebo devices to ensure the validity of randomization during clinical trials.
Data is gathered through various methods, including neuroimaging and biological assays, further enriching the understanding of the therapy's impact.
Discussion and Interpretation
Interpretation of Results in the Context of Existing Literature
The findings from recent studies indicate a favorable safety profile for vagus nerve stimulation. Moreover, improvements in conditions like epilepsy and depression have been documented, aligning with historical observations in the literature.
Implications for Future Research or Practical Applications
The implications of these results suggest that further research could yield techniques to enhance the efficacy of vagus nerve stimulators. Potential extensions of applications could involve treatment for conditions such as inflammatory disorders and obesity. Understanding patient response variability may also guide personalized treatment options moving forward.
The need for comprehensive research is clear, especially in understanding the long-term effects of these devices on neurological health.
"Vagus nerve stimulation is not just about managing symptoms; it’s about understanding the very nexus of mind and body, leading to holistic wellness."
Overall, the exploration of vagus nerve stimulators represents a significant advancement in the intersection of technology and health. The continuous evolution in this field will likely lead to groundbreaking treatments that enhance patient care and open new avenues for scientific investigation.
Intro to Vagus Nerve Stimulation
Vagus nerve stimulation (VNS) represents a significant advancement in neuromodulation therapies. Understanding this subject is crucial given its implications for various health conditions. The vagus nerve is the longest cranial nerve and has far-reaching effects on bodily functions. VNS leverages these connections to influence neurological and psychological health. This introduction aims to establish the relevance of vagus nerve stimulation in medical practice and research.
Overview of the Vagus Nerve
The vagus nerve is a complex structure, originating from the brainstem and extending through the neck and thorax to the abdomen. This nerve plays a pivotal role in the parasympathetic nervous system. It regulates numerous bodily functions, including heart rate, digestion, and respiratory rate. Detailed knowledge of this nerve is essential for understanding how its stimulation affects health conditions.
Vagus nerve also connects the brain to many organs. It influences the heart, lungs, and digestive tract. The diverse role of the vagus nerve indicates its potential therapeutic interventions.
History of Vagus Nerve Stimulation
The history of vagus nerve stimulation dates back to the early 1990s when it was primarily researched for epilepsy control. The first device was approved for use in epilepsy patients in 1997 by the U.S. Food and Drug Administration. Since then, research has expanded to cover various neurological and psychiatric disorders. Scholars and clinicians are continuously exploring further applications in other conditions, which may significantly benefit patient outcomes.
The evolution of VNS has been marked by increasing understanding and technology improvements. Early implementations were limited, but advancements have enhanced the effectiveness and safety of these devices. Continuing research is critical to unlocking more potential uses of VNS.

Purpose of Vagus Nerve Stimulation Devices
The primary purpose of stimulation devices is to modulate neural activity. By sending electrical impulses to the vagus nerve, these devices alter communication between the brain and targeted organs. This may reduce seizure frequency in epilepsy or alleviate symptoms of depression and anxiety. The emerging evidence points to the versatility of VNS, supporting its use not just in epilepsy, but in various other health issues such as anxiety disorders and even migraines.
People with treatment-resistant conditions may find hope in these devices. The ability to modulate complex neural pathways offers a route to manage conditions that are otherwise difficult to treat. It emphasizes the need for ongoing exploration into the efficacy and safety of these interventions.
Anatomy and Physiology of the Vagus Nerve
Understanding the Anatomy and Physiology of the Vagus Nerve is crucial for a comprehensive insight into vagus nerve stimulation. This nerve is one of the most significant components of the autonomic nervous system and plays a pivotal role in many bodily functions. The structure and functions of the vagus nerve underlie the mechanisms through which vagus nerve stimulators operate. By grasping this knowledge, researchers and practitioners can better comprehend their applications and implications in clinical settings.
Structural Overview
The vagus nerve, also known as cranial nerve X, originates from the brainstem and extends down through the neck and into the thorax and abdomen. It has a complex structure involving several branches.
The main features include:
- Cranial Origin: Arising from the medulla oblongata, it integrates into various cranial structures.
- Multi-branching: The vagus nerve features multiple branches that innervate significant organs, such as the heart, lungs, and digestive tract.
- Large Diameter: It has a relatively large diameter compared to other nerves, enriching its functionality.
- Sensory and Motor: This nerve carries both sensory information from organs to the brain and motor signals to control various involuntary functions.
This intricate structural organization facilitates its extensive influence over multiple physiological systems, making the study of the vagus nerve particularly relevant in understanding stimulation therapies.
Functional Roles in the Body
The vagus nerve is integral in regulating numerous bodily functions, reflecting its multifunctional nature. Its primary roles include:
- Heart Rate Regulation: It helps control heart rate through parasympathetic stimulation, playing a critical role in cardiovascular health.
- Digestion Enhancement: By stimulating digestive organs, it promotes peristalsis and enzyme secretion, thereby facilitating digestion.
- Respiratory Functions: The vagus nerve influences the process of breathing, particularly by affecting the bronchial muscles and respiratory rate.
- Mood and Anxiety: Recent studies suggest that it may impact emotional responses, connecting physiological states to mental health.
These functional roles highlight the therapeutic potential of vagus nerve stimulators for various disorders, including epilepsy and depression.
Connection to the Autonomic Nervous System
The vagus nerve is a major part of the autonomic nervous system, which controls involuntary body functions. It forms an essential link between the central nervous system and peripheral organs. Its two branches, the sympathetic and parasympathetic, help maintain balance in bodily functions.
Key aspects include:
- Parasympathetic Dominance: The vagus nerve predominantly activates the parasympathetic response, leading to a state of rest and digestion.
- Homeostasis: Through its broad influence on organ systems, it contributes to maintaining homeostasis, ensuring that bodily functions operate efficiently and harmoniously.
- Reflex Responses: It is involved in various reflex actions, such as the gag reflex and the regulation of blood pressure during times of stress.
The vagus nerve acts as a critical bridge between the brain and the body, shaping both physical and emotional states.
In summary, a profound understanding of the vagus nerve's anatomy and physiology not only enriches the essential knowledge of its functions but also sheds light on the mechanistic basis for therapies involving vagus nerve stimulators. This understanding paves the way for more effective applications in clinical practice.
Mechanisms of Vagus Nerve Stimulation
The mechanisms underlying vagus nerve stimulation (VNS) are essential for comprehending how this therapeutic approach operates and the specific pathways involved. VNS involves activating the vagus nerve electrically to induce various physiological responses that can aid in treating several health conditions. Understanding these mechanisms is critical, as it allows healthcare professionals to maximize the efficacy of VNS devices while minimizing potential risks associated with their use. This section will detail the core principles of VNS, including its operational processes, the different electrical techniques employed, and how the body responds to stimulation.
How Vagus Nerve Stimulation Works
Vagus nerve stimulation works by delivering electrical impulses to the vagus nerve, which is one of the major components of the autonomic nervous system. The vagus nerve carries signals between the brain and various organs, including the heart and gastrointestinal tract.
- Placement: To start VNS, a pulse generator is implanted under the skin in the chest area. A lead wire connects this device to the left vagus nerve located in the neck.
- Stimulation Delivery: The pulse generator sends periodic electrical impulses to the nerve. These impulses stimulate afferent pathways, allowing the brain to respond by modulating neurotransmitters like norepinephrine and serotonin.
- Therapeutic Effects: By altering the activity levels of these neurotransmitters, VNS can have various therapeutic effects, particularly in conditions such as epilepsy and depression. The response varies depending on the stimulation parameters, including frequency and duration of the pulses.
Electrical Stimulation Techniques
Different techniques can be used for electrical stimulation in VNS, each designed to optimize effectiveness and control over the therapy. The following are notable techniques employed:
- Constant Stimulation: This method involves a continuous low-frequency stimulation that maintains a baseline stimulation level.
- Burst Stimulation: This technique uses a series of short, high-frequency pulses interspersed with rest periods. Research suggests that this may be more effective for certain conditions compared to constant stimulation.
- Adaptive Stimulation: Some modern VNS devices include adaptive technology that adjusts stimulation based on the body's physiological responses, potentially increasing efficiency and reducing side effects.
Physiological Responses to Stimulation

The physiological responses triggered by vagus nerve stimulation are complex and multifaceted. When the vagus nerve is stimulated, several outcomes may occur:
- Increased Heart Rate Variability: This is beneficial as higher variability is associated with improved cardiovascular health and resilience to stress.
- Modulation of Inflammatory Response: VNS has shown promise in reducing inflammation in several chronic diseases by influencing the inflammatory reflex.
- Improved Mood and Anxiety Regulation: Stimulation affects the release of neurotransmitters that regulate mood, potentially providing relief for patients with depressive disorders.
"Vagus nerve stimulation represents an innovative approach to treatment, highlighting the brain-body connection and the importance of understanding physiological mechanisms."
Emphasizing these mechanisms not only showcases the potential of VNS but also invites future research into optimizing techniques and expanding applications across various health domains.
Clinical Applications of Vagus Nerve Stimulators
The clinical applications of vagus nerve stimulators are a central focus in the discussion of their impact on health. These devices serve various therapeutic purposes, particularly in treating conditions that have been challenging to manage through traditional methods. As the understanding of the vagus nerve’s role in different physiological processes expands, so does the potential use of its stimulators in clinical settings. It is essential to explore how these applications can benefit patients, address specific health conditions, and the considerations that arise from their use.
Epilepsy Treatment
In the context of epilepsy, vagus nerve stimulation (VNS) emerges as a notable alternative for patients who do not respond to conventional medications. Approximately 30% of epilepsy patients do not achieve seizure control with standard treatment methods. VNS offers a new avenue through the modulation of neurological pathways associated with seizure activity. The device, which is implanted under the skin in the chest and delivers regular electrical impulses to the vagus nerve, has demonstrated efficacy in reducing the frequency of seizures.
VNS provides significant advantages for patients. It is a less invasive option compared to brain surgery. Furthermore, patients report improvements in overall quality of life, including factors like mood, cognition, and physical well-being. Despite these benefits, patient monitoring is crucial due to the possible side effects, such as voice changes or throat discomfort that some individuals may experience.
Depression and Anxiety Management
Another critical application of vagus nerve stimulators is in the management of treatment-resistant depression and anxiety disorders. Conventional antidepressants may not work for everyone, leading to a need for innovative treatment options. VNS has shown promise in clinical studies for patients with severe depression, particularly when combined with psychotherapy.
Research indicates that VNS can help regulate mood and emotional responses. The stimulation alters neurotransmitter levels, including serotonin and norepinephrine, which are vital in mood regulation. Though initial results are positive, the therapy's exact mechanisms remain partially understood, which opens avenues for further research into optimizing its use.
However, it is vital to understand that VNS may not be a first-line treatment plan. Mental health professionals should tailor treatment approaches according to individual patient needs and responses.
Potential in Gastrointestinal Disorders
Vagus nerve stimulation has also shown potential in addressing gastrointestinal disorders. Conditions like gastroparesis and chronic inflammatory bowel diseases may benefit from the use of VNS. The vagus nerve has a significant role in regulating gut motility and secretions, and stimulation of this nerve may promote digestive health by enhancing peristalsis and reducing inflammation.
Current studies suggest that VNS may assist patients with these conditions by improving gastrointestinal function. This application has potential for patients who have exhausted traditional treatments. However, further empirical evidence is necessary to establish VNS as a common therapeutic approach in gastroenterology. To fully validate these findings, extensive trials and research on long-term outcomes are crucial.
In summary, the clinical application of vagus nerve stimulators spans various critical health issues. While epilepsy treatment remains one of the most established applications, their role in managing depression and gastrointestinal disorders shows significant promise. Medical professionals must continue to evaluate and research these applications to maximize the benefits and effectively address patient needs.
Safety and Efficacy of Vagus Nerve Stimulators
The safety and efficacy of vagus nerve stimulators are crucial topics to explore within the field of neurological therapies. Understanding these aspects can inform both healthcare professionals and patients about the benefits and potential risks associated with this treatment modality. Vagus nerve stimulation has been identified as a promising tool, yet it is essential to evaluate its performance and safety profile to determine its overall value in clinical settings.
Current Research on Efficacy
Recent studies have investigated the effectiveness of vagus nerve stimulation in treating various conditions. Much of the focus has been on its role in managing epilepsy and mood disorders. Clinical trials have shown that vagus nerve stimulators can reduce the frequency of seizures in patients with epilepsy. In cases of treatment-resistant depression, evidence suggests that stimulation can enhance mood and decrease depressive episodes.
"The ability of vagus nerve stimulation to modulate brain activity presents a groundbreaking approach in treatment."
Ongoing research aims to understand the mechanisms that underlie its efficacy. This includes examining changes in neurotransmitter levels and alterations in brain circuits that result from stimulation.
Adverse Effects and Risks
Like any medical intervention, vagus nerve stimulation comes with potential side effects and risks. Some patients report localized discomfort at the implant site, voice changes, and in rare cases, increased anxiety. The most concerning adverse effects may include potential interference with other bodily functions, which can be problematic for certain individuals.
Moreover, the long-term safety of the implant itself is under constant scrutiny. Regular follow-ups and monitoring are recommended to track any developing complications. Awareness of these risks contributes to informed discussions between patients and healthcare providers before initiating treatment.
Long-Term Outcomes
Assessing the long-term outcomes of vagus nerve stimulation is essential for determining its overall utility. Some studies point to sustained benefits, with prolonged seizure reduction and improved mood stability for several years following implantation. However, there are still gaps in knowledge regarding how long the positive effects last and how they might vary from person to person.
Ultimately, continued research is necessary to provide a clearer picture of the long-term effects. Implementing strategies to monitor and minimize risks will be crucial as the technology evolves.


The findings in this section underscore the importance of thorough evaluations in safety and efficacy concerning vagus nerve stimulators. It also emphasizes the need for ongoing studies to address current gaps in knowledge and patient care.
Ethical Considerations
In the realm of medical technology, especially concerning devices like vagus nerve stimulators, ethical considerations hold significant importance. These devices, which interact with the body's autonomic nervous system, raise questions that are not merely technical but deeply rooted in clinical practice, access to care, and patient rights. Addressing these concerns is essential to ensure that the advancements in this field are guided by a framework that respects individual rights and societal norms.
Informed Consent in Vagus Nerve Stimulation
Informed consent is a cornerstone of medical ethics. It requires that patients are fully informed about the procedures that will be conducted on them. This includes a clear explanation of the nature of vagus nerve stimulation, possible risks, benefits, and the alternatives available. Patients should not only receive this information but also have the opportunity to ask questions and express their thoughts related to the treatment.
Being informed helps patients make decisions that align with their personal values and preferences. The complexity of the technology used in vagus nerve stimulators can complicate this process. Thus, healthcare providers must ensure that the information is communicated in an understandable manner.
Access to Treatment and Equity
Access to health care is a vital concern. Not everyone benefits equally from medical innovations. Vagus nerve stimulators, often considered for epilepsy or depression, might not be accessible to all populations. Factors such as socioeconomic status, geographic location, and insurance coverage can hinder access.
Here are a few elements to consider:
- Insurance Coverage: Many insurance plans may not fully cover the costs associated with these devices, which can lead to disparities.
- Geographic Hurdles: Patients in rural or underserved areas may have limited access to specialists who perform vagus nerve stimulation.
- Healthcare Literacy: Individuals with limited health literacy may struggle to navigate the healthcare system to receive treatment.
Equity in healthcare is fundamental for ensuring that all individuals have the opportunity to benefit from advancements in treatments.
Future Ethical Dilemmas
As the field of vagus nerve stimulation evolves, new ethical dilemmas are likely to emerge. These could relate to the following aspects:
- Increased Applications: As researchers identify new uses for vagus nerve stimulation, the implications for informed consent and patient understanding will become increasingly complex.
- Data Privacy: Innovations often rely on data collection and monitoring, raising concerns about patient privacy and data security.
- Management of Expectations: With ongoing research, patients may have heightened expectations regarding the effectiveness of treatments, which can lead to disappointment if outcomes do not meet their hopes.
Future Directions in Vagus Nerve Stimulation Research
The exploration of vagus nerve stimulation has advanced significantly But the future directions in this field remain critical for optimizing its benefits. This section highlights the importance of continued research into vagus nerve stimulators in terms of innovation, expanded clinical applications, and the need for translational research efforts that connect laboratory findings to practical medical benefits.
Innovations in Stimulation Technology
Innovative technologies will likely impact how vagus nerve stimulation is administered. Traditional vagus nerve stimulators are implanted surgically. However, researchers are exploring the use of non-invasive methods that could significantly reduce risks and recovery times for patients. Ultrasonic stimulation is one emerging technique that uses sound waves to target the vagus nerve without the need for incision.
Moreover, advancements in wearable technology offer the potential for personalized stimulation. Devices that can monitor physiological conditions in real time may provide stimulation when specific symptoms arise, enhancing treatment efficacy.
This flexibility could lead to more adaptable treatments for conditions like epilepsy and depression, tailoring interventions to individual patient needs.
Exploration of New Clinical Applications
Currently, vagus nerve stimulation is mainly utilized for epilepsy and treatment-resistant depression. Future research aims to explore additional clinical applications, including anxiety disorders, migraines, and inflammatory conditions. Studies are investigating how stimulating the vagus nerve might modulate inflammation, opening avenues for treating autoimmune diseases.
Additionally, researchers are looking at how vagus nerve stimulation might impact metabolic disorders. By addressing glucose control and insulin sensitivity, it may offer new interventions for obesity and diabetes. Such explorations could transform the landscape of treatment options available to patients.
Translational Research Efforts
Translational research is crucial for bridging the gap between theoretical research and practical health applications. This involves validating laboratory findings through clinical trials and ensuring that techniques for vagus nerve stimulation can be adapted safely and effectively for widespread use. Collaboration between neuroscientists, engineers, and clinicians will facilitate this process. It is essential for regulatory bodies to establish clear pathways for new devices and methods that arise from this integrated research.
"Investing in translational research for vagus nerve stimulation could lead to significant breakthroughs in how we approach a variety of neurological and psychiatric disorders."
The future of vagus nerve stimulation will likely hinge on discoveries made through ongoing research efforts. As new technologies develop, clinical applications expand, and translational research becomes integrated into practice, outcomes for patients may improve significantly, making vagus nerve stimulation a cornerstone of modern neurotherapeutics.
Ending
In this article, we have navigated the intricate landscape of vagus nerve stimulators, examining their mechanisms, clinical benefits, and ethical considerations. The conclusion serves as a vital synthesis, pulling together the extensive discussions throughout each section and highlighting the significance of understanding this fascinating field.
Summary of Key Insights
Several key insights arose from our exploration of vagus nerve stimulation. First, the vagus nerve's role in the autonomic nervous system reveals its extensive influence on various bodily functions. Its stimulation can lead to profound physiological effects, which have practical applications in treating conditions such as epilepsy and depression. The electrical stimulation techniques used, while diverse, share a common goal of enhancing the body's responses to restore balance, especially in pathological states. Moreover, the importance of ongoing research is also evident. Without such efforts, the full potential of these devices cannot be realized.
Importance of Continued Research
Continued research on vagus nerve stimulation is crucial. The current landscape of findings underscores the need for deeper investigations into its applications for gastrointestinal disorders and other emerging areas. Furthermore, understanding long-term outcomes and efficacy parameters will continue to shape the clinical use of these devices. Investigating technological advancements will also allow for refined treatment modalities that can tailor interventions to suit individual patient needs, thus maximizing therapeutic benefits.
Final Thoughts on Vagus Nerve Stimulation
Vagus nerve stimulation represents a promising frontier in neuromodulation therapies. As we see more successful clinical applications and increasing public interest, there lies an opportunity to educate and inform both professionals and patients about the potential benefits and risks. Awareness of ethical considerations surrounding access and consent remains critical. The future holds great promise as we harness the underlying technologies and expand our understanding of vagus nerve dynamics. This continued journey can ultimately lead to improved health outcomes and enhanced quality of life for many individuals.







